|
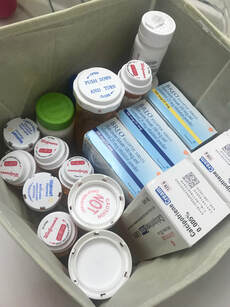
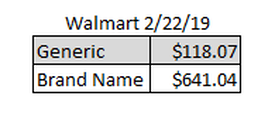
Medical costs are on the rise and, if you're anything like me, can add up in no time at all. I know that I'm not the average patient when it comes to my annual medical spend (I hit the max every year... thank you chronic illness) but even low utilizers can find themselves paying more than they should for medical care. I wanted to take a few minutes today to pass along a few ways to make sure you are getting the best deal on your medications- the bulk of most people's annual medical cost. If you haven't yet read my post about questions to ask before choosing a medical plan please click over as the number one way to save money on medications is simply to understand your medical and prescription drug plan. 1. FSA and HSA PlansFlexible Spending Plans (FSA) and Health Savings Plans (HSA) are accounts you are able to put money into on a per paycheck basis for medical bills on a pre-tax basis. If you have these plans available to you a strongly suggest that you explore those plans and run the numbers in various scenarios as they can save you a lot of money each year. In the case of HSAs they can also let you invest for future health care costs in retirement as well plus both of these plans lower your taxable income which is a plus. 2. Try a Sample FirstWhen you are prescribed a new medication you are typically given a script for a month's supply. Sometimes that new medication simply doesn't work out due to negative side effects or incorrect dosage and the rest of the prescription is wasted as you can no longer take it and have to get a new prescription. This waste- or resources and money- can be stopped by asking for a sample from your doctor before filling th prescription. They can often give you a week or even a month of medication for free to try before you buy as it were. If it works for you- awesome, less money out of pocket for something you love. If not- at least you didn't spend money on something you won't use. 3. Check Your Insurance Program's AppThe insurance program's app is often under utilized. Heading to the app can give you an e-card if you don't have a physical card with you can be helpful but they often have price comparison guides, lists of covered medications, contact buttons, and more just a click away so that you can check before you even leave the doctor's office what your costs are going to come out to (estimated of course). 4. Switch to GenericsGeneric medications are not the exact same formulation as the name brand but they are very similar and depending on your other medications, treatment needs, allergies, and etc. you could very easily be taking a generic form of a medication and see no difference whatsoever- other than big savings. There are circumstances where people are not able to tolerate one generic form of a medication or must take a specific brand name medication and those circumstance would out weigh the financial situation but the chances are that you can, and should switch to generics whenever possible. Example (according to GoodRx): EpiPen 5. Ask About OTC OptionsIf you are on a pricey drug and have seen medications on the shelf at Wal-Mart that claim to treat the same ailment your prescription is treating you might need to switch to that over the counter (OTC) medication. Check with your doctor before making any medication switches as there may be other ingredients or drug interactions that are at play. I am currently on 3 OTC medications that the doctor has included in my daily treatment plan. This does mean that those costs -are not included in my deductible or out-of-pocket max though so I personally pay more per year due to this but I hit that max every year with my medical conditions... for the average consumer this will be more likely to help their budget than hurt it. Run the numbers to find out though and you may even be able to do this in reverse if there is a covered prescription drug rather than the OTC version. 6. Check Your Dosage OptionsJust because the medication is double the strength doesn't mean that it is double the cost. Ask your doctor if the medication you are taking two times a day is available in a scored tablet for twice the dosage. If it is you may be able to split the pills yourself each day and save money. Its important to ask if your medication can be split or not as extended release medications, caplets and some other medications cannot be split safely. 7. Price CompareYou may think that the price of your medication will be the same no matter where you pick it up due to your insurance card but that's not actually true sadly. Your insurance provider negotiates the prices of medications with these distributors so the cost varies by where you get your medications. There are apps out there whose sole purpose is to show you the cost of your medications at various pharmacies so that you can make an informed decision on where you fill your medication prescriptions. Combined with your insurance and any coupons you may have or be able to get through any of the options below you could save a lot of money and even get some medications for free! On this note... you should also ask how much it costs in cash, without insurance when getting medications. Sometimes it can be cheaper without insurance or you can use a coupon you couldn't with insurance to get a better deal. Be aware that going outside your insurance company means that it doesn't count towards the deductibles and out-of-pocket maxes so it may not actually be a better deal long term but depending on your situation it could save you money to go this route. 8. Mail Order/Bulk DeliveryOften times you can get a discount on the medications you take every month by having your doctor write you a script for 90 days rather than 30 days. You can have this 90 day prescription filled by an online pharmacy and shipped directly to your house saving you money on gas as well as the cheaper-per-dose prices for ordering in bulk. I typically use the one my insurance recommends but there are cheaper alternatives sometimes... just be very careful if you do this to verify the legitimacy and legality of having that particular pharmacy ship you your medications. 9. Coupons & Patient Assistant ProgramsBet you didn't know you could coupon medications. You totally can! Not every medication has a coupon or program available but a quick Google search of "Medication + Coupon" or "Medication + Patient Assistance" could net you big savings. I personally am enrolled in a program that pays most of my costs for a medication that costs over $2,000 per month up to $10,000 per year as well as using a coupon for my annual Epi-Pen (generic brand, of course). I have also had coupons for free inhalers and other medications. Many of these coupons and programs have requirements and stipulations (such as being under a certain income, having or not having a certain type of insurance or etc.) and an approval processes but taking the extra time to fill out the forms could save you hundreds or even thousands of dollars each year. The coupons might get you a discounted rate on the medication, a rebate for your medications if you mail in the receipt, or even free medication for a limited time. Most of these are from manufacturers so you do have to get the exact brand which isn't always the easiest to do but its worth it. My pharmacy is special ordering the generic Epi-Pen that I have a coupon for so that I can get the lowest possible price for my necessary medications, it will take a few extra days or maybe even a week but I'm willing to wait as those savings add up. 10. Prescription Savings CardsThis one is one that I will tell you to be careful with. While you can save money at point-of-sale for your medications potentially you may be going around your insurance plan to do so. Doing this means that it isn't being counted in your deductible and out-of-pocket amounts so, like moving to OTC medications, it may actually cost you more in the end if you are going to be getting up towards that out-of-pocket maximum amount by the end of the year so run the numbers and make sure you're making the best decision before you do this. Some cards don't go outside the insurance and work the same as a coupon though... just be careful and ask the Pharmacist to explain all your options and how it will interact with your insurance plan before choosing this option. 11. Pharmacy Discount PlansPharmacies are always trying to get customers in the door and need repeat business just like any other business so they often will have discount programs for their customers that they run... especially big-box stores like Kroger and Wal-Mart. Wal-Mart has a $4 prescription plan for instance for a 30 day supply of medications for a list 2 pages long. If you are taking one of these medications then it would be a good choice to consider them for filling it. They make money off the other medications you fill with them as a repeat customer so it makes sense for them and it makes sense for you as its cheaper. One thing to note here is that if you are getting medications at different pharmacies you should make sure that they all know all medications you are taking. If they don't they can't give you important information about drug interactions or valuable suggestions on alternative options. They may even be able to match price with the pharmacy you are getting your other medication from if you let them know that's why you aren't getting all of your medications from them. 12. State Subsidies and Other Care PlansDepending on your situation you may qualify for additional assistance from the federal or state government. If you think this could apply to you it is important you reach out to to their assistance agencies to find out if you qualify. These programs are often limited to those in lower income brackets, on other assistance programs, enrolled in Medicare or etc. but looking at all of your options is an important part of advocating for the best possible care you can get. 13. Talk to Your Doctor...If you have a question about why you are being given a specific medication or if there are alternative options then the best person to ask is your doctor. Being open with them and discussing the financial implications of your treatment plan is the first step towards being an informed, involved participant in your own care which is what we all should strive to become. If you let your doctor know that X medication is higher priced than you can afford and ask for alternatives they can help. Often they are not aware of medication costs as they are not involved in the negotiations your insurance company has annually with drug manufacturing companies, but once they are aware they can help you find an alternative treatment option that is a better fit financially but also works for your health management. 14. Ask Your Pharmacist...The last tip today is simple to ask the pharmacist: is this the cheapest option? They may know of a coupon or other discount that can save you money on the spot. Don't...
I've been wading through this costly medical system most of my life but hopefully you won't have to waste as much money as I'm positive I did over the years while still learning about these options with these tips. Until next time, Formulary, Preferred, Generic, Name Brand, Off Label, Pre-approval, Copay, HDHP, PPO, HMO... there are so many possibly unfamiliar terms when it comes to medical insurance. When you are signing up for a medical plan, whether through your employer or the market place, it is imperative that you make yourself an informed consumer. This means taking the time to understand all the ins and outs of the plans available to you and your family. If you are choosing insurance through your employer the Human Resources department can be an invaluable resource for you. They know the ins and outs of your plan(s) and if they don't have an answer to a specific question they can often give you the number of someone who will. It is important to remember that they are still your employer and coworkers so you may not want to share ALL your medical information with them but they can help to explain your plan options in broad strokes so that you can chose the best plan for your family. A few things to look for: What pharmacies and providers are in-network?Never ask a provider if they 'take' or 'accept' your insurance- the answer will likely be yes- you want to know if they are in-network. I'm not completely jaded and understand and even trust that most providers will be up front with me if I mess up and ask if they take my insurance but I was burned once, badly, and learned my lesson so no longer do this. In my case I was lied to by a front office staff member at an Urgent Care center and spent the better part of a year fighting about those out-of-network costs with the provider and my insurance company, it was not fun. If there is a provider that it is important that you see then you should call the insurance company and ask if they are in-network before you sign up for a plan and double check with your insurance company before going to a new provider. Going out of network can mean significantly higher costs not just for your specific medication or visit but for the whole year as you have separate in- and out-of-network deductibles and out-of-pocket maximums. It may look something like this: Are there Preferred pharmacies?This can often save you money as well. You will often see this affecting you when it comes to co-pays and co-insurance so it never hurts to ask. Going across the street could save you 10%! What is my deductible?Is there a per person deductible or per family? Does it include prescription medications or is that a separate deductible? Some plans will have a separate prescription deductible that you will have to meet before medications reduce in price or become paid for. This deductible will typically go towards to you out-of-pocket maximum just like your medical deductible but its important to know if you are going to be juggling multiple deductibles. What is my individual and family out-of-pocket maximum?If you have one high utilizing family member then its important to note that often plans will include a per-person cap that can keep your costs lower... you many not have to get all the way to the family out of pocket max to stop paying for that person's care for the year. This can be a lifesaver when it comes to the budget. What medication are formulary or covered?Check the plan every year, even if your plan has not changed, to make sure that all your current medications are covered. Insurance companies issue a new list of changes each year and you can often find this on the website but if not then simply call in and request it. How does the co-insurance work?Once you hit your deductible you will often still be responsible for some of the costs until you reach a higher number, the out-of-pocket maximum. This is usually calculated at a percentage. So if you have a co-insurance of 80% once you hit your deductible that would mean that you are responsible for paying 20% of the cost for your care until you reach that number. In and Out of Network still apply for this portion of your yearly cost so its important to stay in-network if at all possible. What are the requirements for Specialty medications?For certain medications, typically higher costing medications and ones that require temperature control, some plans will require you to use their Specialty Pharmacy in order to get them filled. This saves them money which in turn saves you money in the long run but it can be a little frustrating to have to schedule delivery for these medications and call in your payment/authorization to ship each month. If you have a medication that falls under this type of requirement they will let you know when you try to fill it at a retail pharmacy but if you think it may apply to your situation it could speed up the process to simply call the insurance company to ask up front what their policy is in regards to that medication. Processing at these pharmacies takes much longer than your corner CVS so planning your doses out is imperative for these kinds of medications. How do Prior Authorizations work on this plan?Certain medications, treatment plans, surgeries or even provider types may require Prior Authorization in order to be covered. These will typically span a length of time and then require renewal if it is an ongoing treatment. This is a pain to go through and number two cause for my personal medical plan headaches but its important to understand and follow this process or you could end up paying the full cost of treatment as the charges will be denied. I am personally on a medication that costs over $2,000 per month for me to take... you can bet it requires Prior Authorization. Every 6-18 months (depending on how long they authorize the treatment plan) my doctor's office has to file paperwork showing that I still need the care. Sometimes its easy but other times its a fight. Sometimes its just not worth that fight and we will chose an alternative treatment or I will pay out-of-pocket, like i did for my current rescue inhaler. Being prepared for this process and not letting it frustrate you if important- the insurance company is trying to keep their costs down by verifying that the treatment is necessary which helps keep costs from rising even more for everyone. What do I need to do in order to see a Specialist?For some types of plans all you have to do is show up to receive covered care but for other you may need a referral. Knowing this up front will save you headaches and money from fees for seeking care without a referral. Is ____ covered?If you are looking for a specific type of care then ask up front if it is available on plan and if so how many sessions/how often you are able to get it. A good example of this is chiropractic care. Some plans offer it but they may limit the number of sessions you are able to have covered per year. Other options could be infertility treatments or in-home care. If its not then you may need to purchase supplemental insurance or go with a different plan. Are there any perks to the program?I am with Blue Cross Blue Shield of Texas currently and there are a ton! My plan includes an identify theft program, a gym membership discount plan, teledoc services, free coupons to all kinds of health related retailers, discounted magazines, a wellness points plan and even discounts on services they don't cover like acupuncture and massage at certain providers through one of their free programs. On the wellness plan I get points for doing things like going to the gym, taking an online class, entering my stats quarterly, and etc. which I can exchange for prizes like kitchen gadgets, gift cards, and more. You can bet I participate in this when I have time... a few minutes while waiting around gets me a little closer to a free blender. :) Does this plan qualify for a FSA or HSA? If so is one offered?Flexible Spending Plans (FSA) and Health Savings Plans (HSA) are two ways that you can pay for medical costs with pre-tax money. They both have their own requirements as well as good/bad points but having access to pre-tax money can save you quite a bit of money. I'll do a separate post on these plans but if your employer offers them please learn about them and utilize them. They may also have a Limited FSA just for Dental and Vision, a Dependent Care FSA to help pay for childcare expenses pre-tax or an Health Reimbursement Program (HRA) that, while it isn't tax free, is free money to help you meet your medical costs if you submit for it. All of these plans are going to be employer specific in whether they are provided and through which providers but making sure to really understand your benefits package is an important part of providing health care for your family and being an advocate for your own.
I hope this helps you navigate your medical insurance journey. Until next time, It’s difficult to explain how important it is to lower my monthly expenses by paying off my student loans- as well as other debt- without explaining where a huge chunk of my annual income goes without any real choices… my medical expenses.
For someone like me who has chronic illnesses, maintaining health insurance coverage can literally be the difference between a fairly normal life and absolute destruction. I make the joke that I work for health insurance but to be honest it’s not much of a joke. According to BCBSTX the billed amount for my medical expenses in 2018, a really good year for me with only one chronic illness really causing problems rather than all three, was $46,823. That’s a full time salary for many in the US and it doesn’t even take into account costs that I incur outside of the insurance plan for uncovered medications and services. In order for me to ever be fully financially independent I need to eliminate as many of my monthly debt payments as possible while also building a large emergency savings so that in the event of a job loss I could afford to maintain my healthcare costs without going bankrupt. For this reason, I thought taking you through a summary of my anticipated costs for 2019 would be helpful. So here we go. First, some important terms then a summary of this year’s insurance plan and then a quick run through of additional costs. This post is part of a series that will look at ways to save money on medication, questions to ask your HR representative during Open Enrollment season so that you can make an informed decision and more. Insurance and healthcare are, understandably, a huge passion of mine which I have only dug deeper into since beginning to work in Human Resources four years ago. I hope that this series can be beneficial to you. Important Terms
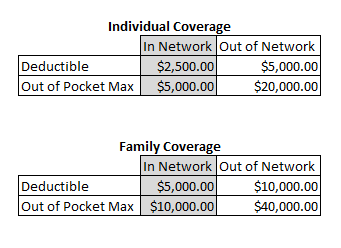
My Insurance Plan I currently have a fairly good plan but it is a High Deductible Health Plan which can get very costly if not budgeted for and fully understood. Being an informed consumer is of utmost importance with this kind of plan as 100% of the cost for services is on you from day 1 until you meet the deductible. Here are the details for my exact plan:
My insurance plan does not cover two of my currently prescribed medications (up from one in 2017) or any of the over-the-counter medications that my doctor utilizes as part of my treatment plan. This part is standard though, no prescription drug plan will cover OTC medications as a rule and have exclusions for covered prescription medications. Since this particular medication is purchased at a compounding pharmacy is was pretty much known up front to be an uncovered expense. It also doesn’t cover some of the testing I have to do at my allergist/immunologist’s office when I am in a flare, vitamins and minerals that I supplement with when symptomatic, or any of the alternative treatments that I have found helpful to maintaining my health. While it is true that most of these costs boil down to personal choices that I have made to seek these treatments the quality of my life has increased drastically since introducing them so keeping them in my treatment plan if possible is ideal. Not Covered Costs Breakdown
Without any of the ‘not covered treatments’ category we’re looking at:
Other Costs One thing that isn’t accounted for in any of these numbers is the fact that I have to be careful about the foods that I eat and products that I use. I am allergic to a lot of things- most artificial scents, gluten, celery (random I know), bananas, and a slew of other things. This translates to needing to use more expensive personal hygiene and cleaning products in many cases as well as having a more heavily padded food budget than your average single person. I wish I could discount this but its part of my life and relates directly to my health issues so it likely should be mentioned. In my house you will find no scented candles, plug-ins, or etc. as they trigger migraines for instance and just this past Christmas I borrowed some basic laundry detergent while on vacation and was covered in hives for three days… so you can imagine a lot of shampoos, detergents and etc. can ruin my week pretty easily. Ways I Lower My Costs
I write all this out not to convince you to feel sorry for me or what have you, because I think that I am extremely lucky to be able to work at all as I have many friends who are not able to do so. And not only that but I have a job I love, that pays me enough to afford the life I have- including insurance and salary that can encompass these expenses, a life that’s amazing with hobbies that bring me joy and friends that bring light and happiness to it, and a family that is just without words wonderful. It’s more than I deserve and I will always be grateful for it all. I write this to show you a window into my life for better understanding of one of my largest “why’s” when it comes to becoming financially independent and debt free. Having a “why” for your goals is important as without one you will be more likely to convince yourself out of the hard but necessary tasks along the way towards reaching your goal. Until next time, So a completely unexpected thing happened the other day... I got another diagnosis to add to the intake form. New diagnoses aren't something I fear anymore. After all, no matter how scary the name, a diagnosis doesn't change my symptoms for the worse just by existing. Sometimes the new meds that come along with it can cause a hiccup in my life for a while, sure, but in the end knowing can only lead to potential help from my point of view. Knowledge is power and having a name for something means that there is likely research and papers out there that could potentially improve my life.
I'm pretty used to diagnoses taking years to get at this point. That's how it's always been for me, my first dysautonomia diagnosis took 6 years! That's actually pretty average for that group of disorders too in case you're thinking "that's CRAZY!" The other day though... hours, mere hours. The diagnosis: MCAD. It was exciting to speak with a doctor who actually understood what was going on in my body rather than just in the one area they look at... and she brought a hope for a brighter future that I haven't really had in a long while back into my life. Dr. G thinks that treating my MCAD can help everything from my migraines and pain (it may not be fibromyalgia after all!) to my dysautonomia and asthma. She didn't promise a cure for all of my ills but she did provide hope for lessened symptoms over time rather than the understanding that I've been living with: that I would get worse over time and there wasn't much I could do to stop it. When I made an appointment with Dr. G I didn't expect anything, not really. I was hoping that this pulmonologist that I had found on Google- because she was open on Saturdays and I didn't want to take any more time off work in case I needed to go back to the neurologist- would at least treat the asthma that had been flaring up more than normal and maybe find a new allergy medication for me since the one I was one seemed to be barely helping at all. I resigned myself to likely needing to go back on oral steroids and just hoped that when she saw my intake form she wouldn't write me off as having a Somatoform disorder and send me on my way. It's a real fear guys. Once you're labeled 'officially' as having it all in your head doctors stop listening. As soon as it touches your health record it's so hard to get things done for you, necessary things... like medications that keep your heart rate in check or a check to see if your electrolytes are out of balance when you head to the ER because you can barely stay awake. Thankfully I only have had doctors say it out loud to my face ("I don't believe in that disorder." Seriously Doc? I have, in my hands, more than a decade of medical records that you are dismissing because you 'don't believe' in a known, researched and many times published medical condition... yeah, patient advocate time.) but never bother writing it down. This is not the case for many patients that I know... they have to fight with hospitals and doctors to get a note added (but the old note remains) that the previous note was incorrect. Side note: Those intake forms where have you check all the boxes of symptoms that you have experienced in the past 3 months are the bane of any Spoonie's existence. 'Normal' people might check that you've had several headaches, sinus issues, and one or two other things then check off a family history of diabetes and be done. We have to check nearly single every box... and hope that they take us seriously when they see all the side scribbles and notes on the margins trying to explain why there are so many and that we aren't hypochondriacs. Hypotension- check- Monday afternoon 96/60 Hypertension- check- Tuesday afternoon 160/101 Heart palpitations- check- also on Tuesday Tachycardia- check- Monday evening 135, standing Bradycardia- check- Monday morning 54, sitting Nausea- check- Monday evening, likely due to tachycardia Digestion issues- check- IBS, cycles Dizziness- check- related to dysautonomia Vertigo- check- related to dysautonomia Headache- check- migraines, tension headaches, sinus headaches; being treated by Dr. Y Trouble breathing- check- this is why I'm here Sinus trouble- check- also why I'm here Joint pain- check- referral out from Dr. Y to a rheumatologist check, check, check, check, CHECK! "When everyone is super, no one is"... the same goes for symptoms. If they're all checked then doctor's have no idea what is actually important, they don't know where to even start. Don't even get me started on the 'Medications & Supplements' area... two lines, really? Diagnoses and surgeries... I need my cheat sheet for all those dates. But I can spell everything for you when your nurse asks me about it all to put into the computer in 15 minutes. It takes forever and is pointless because you just have to go over it all in context when they come in for your little bitty time window appointment. *end rant* Anyways, Dr. G didn't do any of that... exactly the opposite actually! I gave my information to her interns (who had growing eyes and lots of questions for each thing on my list... they must have been new) and as they were filling her in on everything I had told them she made a few hypotheses. The first was that, despite being on anti-histamine drugs for years and having taken a dose less than 24 hours before, I would test positive on a histamine test. The nurse tested me and, of course, a nearly instantaneous positive result came from the test. I didn't realize it at the time but that's not supposed to happen for normal allergy sufferers apparently. In her consult she made sure to let me know why she wanted the test and what it meant. This was my first inclination that I had stumbled upon someone who could, and would, help... she didn't guess and medicate, she made hypotheses and tested them before doing anything further. Next up was a Pulmonary Function Test and a diagnostic form to verify that my asthma wasn't under control. Again, unsurprisingly... it wasn't. The first consult happened next. She brought the hypothesis forward that I had MCAD and gave her reasoning and plans to verify this hypothesis. Based on my history (I was very general on the forms that I filled out because I figured it would be more likely that those in the office had heard of the general category of disorders rather than the specific subsets. I should have just put the specifics down to begin with but I'm a bit jaded I suppose...) and the few tests she had run already she managed to identify nearly all of my specific diagnoses as well as some that are still in unverified status but highly likely. We were able to discuss my symptoms from ALL of my diagnoses and how they interrelated and how MCAD could be affecting my body and it's disorders. A real conversation... if you don't have a chronic illness you don't understand the relief and joy that comes from meeting someone who you can speak with about what you go through without having to 'dumb down' or explain everything. Not to mention the anxiety and fear that you'll somehow scare them away from you- doctor or friend alike on this one. I was nearly giddy by the time she left the first time! I had to call my mom and let her know that the quick appointment I had anticipated was going to be quite a bit longer and so much more fruitful. Apparently I had stumbled upon the doctor that I would have eventually ended up at once I got back to a dysautonomia specialist again... she works with people like me all the time! There are really no words to explain what I was feeling at this point... relieved, excited, giddy, happy, optimistic... none quite fit yet they all do. I know what I wasn't though- scared or anxious. She wanted to do an allergen test next. That cost a pretty penny but I haven't had one since I was a child and that was prior to having years of allergy shots as well as moving around the world so it was, needless to say, rather outdated. It was... less than fun. This will sound like a complaint but it's just a run down of the next hour or so. We started with the test on my back. The little needles stung and I itched for pretty much the entire next few hours but if it helped make me better I was all for a little pain. Like my massages, they hurt at the time but they help so I say go for it. Lying on my front also caused my ribs to have significant pain so lying still wasn't 100% possible but we found a way to make it work. I was pretty glad when that was over to be honest and hopped right off the table to get dressed. Hopping directly off the table wasn't my best choice but I was excited for answers and completely forgot about managing my POTS so ended up grabbing a wall as the room spun around me for a bit at that point. A rest lying down was necessary but and I was able to move forward by my next consult time. I still make silly mistakes that cost me time and energy all these years later. It's rather annoying but its part of being human. :P The final consult consisted of figuring out a plan of action- together. She placed an order for some lab tests (which she's going to personally call and discuss the results with me... who does this anymore!?!) as part of the next step in finalizing the diagnosis. Then we discussed whether I wanted to go straight to medicinal treatment or try some more natural approaches to desensitizing my mast cells first. I'm all about natural methods and staying away from the more dangerous or long lasting medication when I can so I'm super psyched that she is as well. There can be so many interactions when you're being prescribed many different meds but many different doctors... its hard to tell sometimes what caused what and if a treatment plan is actually working. For this reason, we ended up deciding on a mixture of natural and medicinal for the next few months. I'm on allergy and asthma medications, which are necessary for me at the moment, plus I started an elimination diet to start the process of lowering my histamines and finding out what causes issues for me. I'm not going to lie, it sucks. She gave me a bare bones list of items to avoid and told me to try to stick to a low histamine type diet as best as possible until I came back in. I threshed it out a bit more because I'm me and needed to understand the why and do's/don't's better. What I ended up with was a low histamine diet mixed with AIP basically. I do best symptom-wise on Paleo and when you add in a histamine intolerant diet to that mix it gets pretty restricted in the flavor area... at least it seems that way for a big fan of cooking like me. In 6 weeks I go back to discuss how the diet and meds have helped and we will look at beginning at the next step of my treatment plan. Hopefully that will include adding in some of the foods I've cut out as I already miss cheese and salsa something major. I came to terms with my health years ago. A lot of the time it's felt like a fight to stay where I am rather than a fight to get better, at least in recent years. The IBS issues and tachycardia would improve with trying this new thing or that but then the pain would get worse. A new medication would cut my migraines in half but made my heart rate unstable so I couldn't exercise. I've gained weight, pain and exhaustion the past few years despite gaining some ground on the nausea, tachycardia and IBS issues. Don't get me wrong, I'm in a much better place overall than I have been in the past medically speaking. I have a fairly normal life (and I can remember a time when that seemed to be going away) with friends, work, & hobbies. I'm very blessed and I know it... but I stopped praying for someone to find a cure. I started instead praying that I wouldn't get worse like so many of my friends have. Eventually I stopped asking at all about my health. That doesn't mean that I stopped treatment and just stayed home depressed and miserable, I didn't. I kept fighting and I always will. I just found some good in the bad that I have experienced... I found peace in being who I am and stopped dreading the future so that I could fully live in the present. Now? I'm still sticking with that outlook of peace and trying to live each day that God has given me to the best of my ability... but there's hope, and prayer, for a brighter future than the one I had resigned myself to. I've had allergies and asthma since I was a kid that caused some issues but my chronic illness journey didn't really start until I was 12 years old. In October of that year I was hospitalized for a week when I needed an emergency appendectomy. I came in to the ER with a pain, a high fever and, unbeknownst to us, pneumonia and ended up in surgery fairly quickly to have my appendix removed. A fairly standard operation ended up keeping me in the hospital for a week as my fever shot up very high every evening as I healed from both the surgery and pneumonia. Everything seemed fairly normal after I left the hospital though, I was very tired and couldn't do a lot of exercise but that was to be expected. Over time when the fatigue didn't abate and I started getting more symptoms, such as high heart rate when I was standing, dizziness, vertigo, and nausea, we went to our family doctor trying to find answers. It didn't even occur to us that it was side effects from the surgery since it had been quite a long time by this point and I was healed. In truth the surgery and ensuing hospital stay wasn't the reason that I was sick but it was, most likely, the trigger that set everything else in motion. When you have dysautonomia it isn't a disease you catch but rather something you are predisposed to developing.
The journey to find answers to the mysterious illness that was slowly taking over my life took 6 years and included several cardiologists, a pulmonologists, a gastroenterologist, a sleep therapist, a couple of neurologists, an endocrinologists and even a psychiatrist when they thought that maybe depression was causing the insomnia and possibly more. The therapist sent me home with us both in agreement that I wasn't depressed. At points later I will admit though that depression did come into play in my life but it wasn't the cause of my illness(es). Symptoms ranged from gastrointestinal issues like IBS to heart problems such as tachycardia and blood pressure spikes/dips and more but it seemed like no one had the answer to what the diagnosis should be. There were some wonderful doctors along the way who cared very much and did their best to treat the symptoms I was experiencing and then there were some doctors... we'll just leave it as they weren't so wonderful in their treatment of me. Eventually I was diagnosed with POTS, NCS, and NMH. All three are forms of dysautonomia which is a disregularization of the autonomic nervous system. Having a diagnosis didn't really change the treatment I was receiving very much though as, at the time, treatment was mostly symptom management which was what we were already doing. However, it opened the door to support groups around the world that were all dealing with the same issues as me. That was a blessing beyond measure. Over the years my symptoms have had good spells and bad spells but I know so many others with the same conditions as myself who are in much more difficult situations medically. I am very grateful that I am able to work for instance- I can't work outdoors in the heat and I can't do a lot of physical labor type tasks but I can work in an office or a classroom. I am grateful that I am able to walk- not everyone with dysautonomia can stand for more than a few minutes, let alone walk far. My limit used to be 20 minutes for standing which made regular activities such as grocery shopping, going out with friends, and getting around an airport rather tricky to say the least. As I have found physical coping mechanisms, changed lifestyle habits, and perhaps just gotten better somehow, I have been able to reduce a lot of my symptoms and I can stand for much longer now. Within the past few years a few new things have come my way on the medical front. A diagnosis of MTHFR, a genetic disorder that affects detoxification and menthylation within the body, was one that came on the heals of a scary time for my sister. She had some issues and the doctors discovered that MTHFR was the problem. Since it is genetic the whole family needed to be tested. I had to fight for a year to be tested as they told me there was no cause to test because there isn't a treatment and that it 'really doesn't cause any problems.' So far research has linked blood clots, aneurysms, miscarriage, depression, fatigue, migraines, certain mental disorders, anxiety, high blood pressure, and other issues to MTHFR- some of which I experience myself. This does not mean that MTHFR is the cause of these issues though, further research is needed to determine causation, as of now we only have a link or association. I have defects on the two main genes they test for when checking for MTHFR but I only have one copy of the mutation on each gene rather than two (this would be called compound heterozygous) so my symptoms aren't as pronounced as someone who would have both copies but worse than someone with no copies or a copy on just one gene. The second issue that has come up is pain... All of the pain. Every morning I wake up and roll out of bed hearing a dozen snaps, crackles and pops in the joints of my body. They usually do not hurt much but if a joint subluxed, or partially dislocated, while I slept there is pain. The joints that are more common for me to sublux in my day-to-day activities are my hips and shoulders but my ankles roll regularly and my knees give way without warning as well. Recently my thumb has begun to start subluxing more often as well... that isn't particularly fun but it will eventually be just like when my hip or shoulder does- put it back and move on with my day. All the pops and cracks along my spine especially tend to mean pain and inflammation. Luckily I have a wonderful massage therapist who I see regularly to help with the knots and tension that inevitably occur from all of this. Without her I would likely be dependent on pain killers and anti-inflammatory meds which would be bad for the next issue I'll talk about. I'm still waiting to be seen by a geneticist but symptom wise (there are more but this post is getting really long so I'm skipping past them) I'm likely looking at a form of EDS. The last issue that I've been dealing with lately is headaches. I pretty much live with what I now consider to be a low grade headache 75% of the time. Sometimes that low grade headache will go away (hurray!) but other times it turns into a migraine, higher intensity tension headache and even the occasional cluster headache. I am working with a neurologist to see if we can discover the cause but so far we have ruled out rebound headaches. I have an MRI later this week as well as an ophthalmologist appointment upcoming to check for some of the worst issues like swelling in certain areas of the brain, descending cerebellum and tumors. After the doc looks over the results I may be looking at a spinal tap as well (no fun...). I am hopeful that we can find the answer and if not fix it then at least find some ways to combat it. That's a pretty quick overview of the last 15 years of my life from an illness perspective. There have been a lot of bad things but also a lot of good... I wouldn't be who I am today without having gone through everything that I have in my life. I like who I am so it makes the good list. Further, I have met some amazing people on this journey that I wouldn't have met otherwise. I've been able to help people that I may not have been able to otherwise. I also discovered Paleo/Primal/Real Foods Movement along my journey... it has changed my life for the better. My symptoms are so much better and it has opened new doors to my understanding of my body with researching the diet and lifestyle that surrounds many of its practitioners. Basically... it's not all bad, I'm used to a certain level of pain and live a fairly regimented life most days but it is who I am and I am ok with that.
I am currently reading Wheat Belly: Total Health by William Davis. I'll post a review once I am finished reading the book but so far I can say that this book is jam-packed with more information than I will be able to fully absorb in a single read so if you are looking for a comprehensive text on the history of grains and how they interact with the human body this may be your book. Since I was spending so much time delving into the complexities of wheat as a food stuff I was wondering how much my avoidance of wheat was truly the reason I was feeling so much better as the book states... so I posed an experiment. I re-introduced grains for one week, 7 full days. I made sure that I was keeping as many other factors the same as possible within my diet but I added in bread and other grain products. For instance, when I ate a hamburger I ate the bun instead of my usual bun-less burger. I didn't go crazy and change my diet 100% back to the Standard American Diet, just a few servings of grains per day. All in all the week went exactly as I expected... here's the breakdown:
Monday: I reintroduced wheat by choosing a small portion of mushroom stuffed ravioli at lunch but kept everything else the same in my diet. I felt more tired that evening and had a touch of the insomnia I had previously kicked while being grain free. Tuesday: I had a biscuit at breakfast and a slice of pizza at a work gathering at lunch but dinner stayed the same as usual and was nearly carb free as I was feeling pretty poorly. My stomach began acting up and I started to bloat. Wednesday: My POTS started acting up with tachycardia and nausea. I also had to take some headache medication and was exhausted by the time I came home from dinner. I did not have grains with lunch or dinner, only at breakfast. Thursday: Still feeling poorly in general, my stomach was still acting up- IBS was back in full swing- and I needed to lie down at work for a few minutes as I had a tachycardia attack with nausea and vertigo. I didn't make it to my after work activity (choir) as that was out of the question... I simply went home to lay down on the couch. Friday: I had been noticing that it was more difficult to think as clearly this week but now it was quite pronounced. I could only read a few pages at a time without a break today as I typically had to re-read sections to fully comprehend the complex subject matter of my grad class. I fell asleep early tonight. Saturday: Today was a bust... I woke up with a migraine which meant that I didn't move or do much of anything until well after lunchtime and then was exhausted and still in pain/nauseous for most of the day- even with 3 different migraine/pain medications. For this reason I ended up ordering a pizza and calling it a wash- I was already on the eating grains bandwagon for two more days and it was easy to be honest. I have been craving sugar like it's nobody's business since about Wednesday as well I realized. Sunday: Since I fell asleep at nearly 4am due to the copious amounts of sleep I got on Saturday and the physical and mental exhaustion that has been the week in general I missed church in the morning. I was still sluggish for most of the day and trying to do homework was ridiculous in the evening. I was looking forward to stopping the grains again on Monday but not looking forward to the possible withdrawal symptoms triggered by coming back off the grains. Symptoms that came back on grains:
If you are interested in purchasing Wheat Belly: Total Health I am including a link below. Your local library likely has several books on Paleo and grain-free living as well. Happy reading! |
Details
Archives
October 2022
Categories
All
|

 RSS Feed
RSS Feed
